Amir Abbasi
Falls are one of the leading causes of injury among older adults, but what many people don’t realize is that the heart plays a major role in fall risk. When the heart isn’t functioning at its best, it affects blood flow, blood pressure, energy levels, and balance.
For seniors already managing heart conditions, understanding this connection can be life-changing and potentially life-saving.
Having the right mobility support in place is one of the most practical steps a senior with heart issues can take. Our guide on Best Walkers for Seniors with Balance Problems is a great place to start when looking for the right stability aid.
Whether you walk daily for fitness, spend long hours standing at work, or simply want safer movement, understanding shoe structure will help you make an informed choice.
Table of Contents
How the Heart and Fall Risk Are Connected
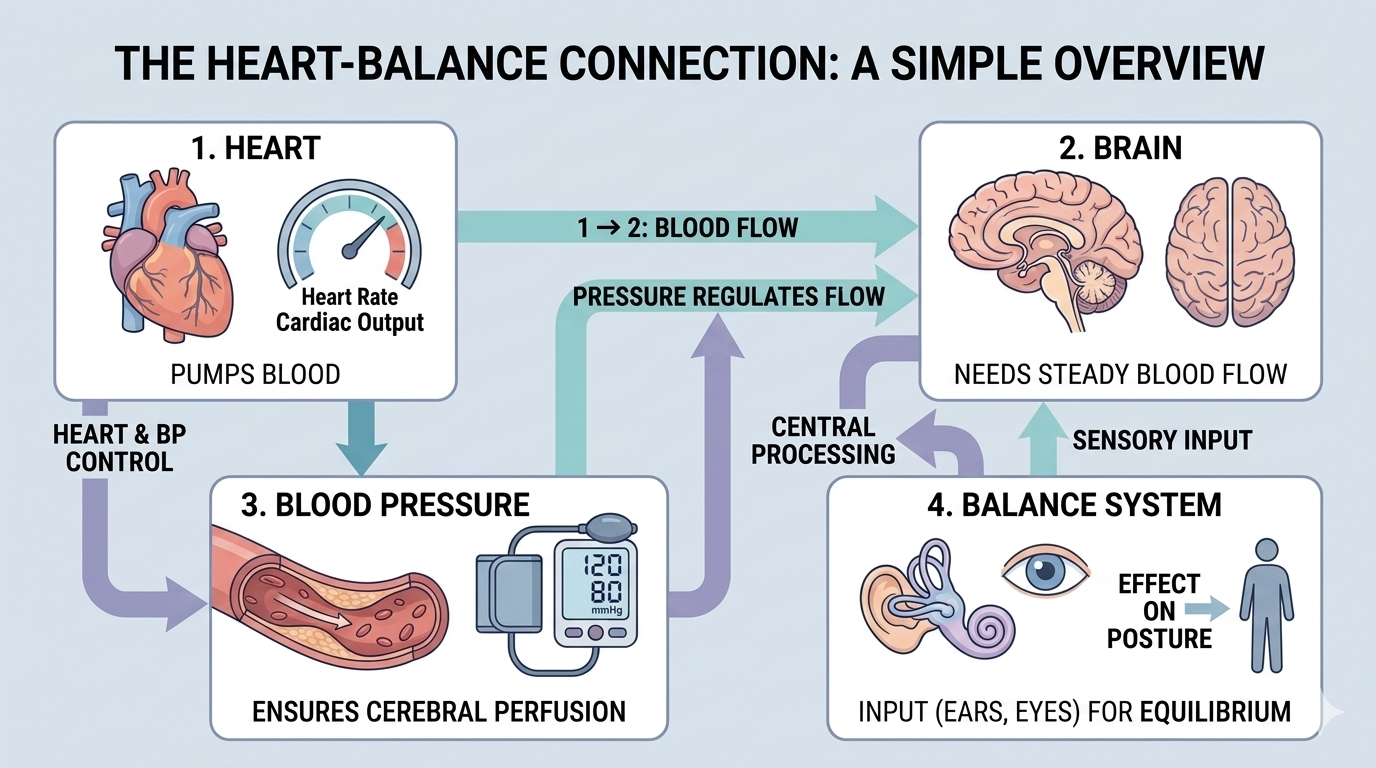
The heart is responsible for pumping oxygen-rich blood to the brain, muscles, and every organ in the body. When that process is disrupted, even briefly, it can cause dizziness, weakness, confusion, or sudden drops in blood pressure. Any one of these symptoms can cause a senior to lose their footing and fall.
The relationship between heart health and fall risk is not always obvious because the symptoms can be subtle. A senior might simply feel “a little off” or suddenly lightheaded before a fall occurs, without ever connecting it to their heart.
Heart Conditions That Increase Fall Risk in Seniors
1. Orthostatic Hypotension (Low Blood Pressure on Standing)
Orthostatic hypotension is one of the most common causes of falls in older adults. It occurs when blood pressure drops suddenly after standing up from a seated or lying position. The brain temporarily receives less blood, causing dizziness or lightheadedness that can result in a fall within seconds.
This condition is frequently linked to heart disease, dehydration, and certain medications.
2. Arrhythmia (Irregular Heartbeat)
An irregular heartbeat means the heart is not pumping blood consistently. This can cause sudden feelings of weakness, palpitations, fainting, or brief blackouts, all of which dramatically increase fall risk.
Atrial fibrillation (AFib) is one of the most common arrhythmias in seniors and is strongly associated with falls and related injuries.
3. Heart Failure
Heart failure doesn’t mean the heart has stopped; it means the heart is not pumping as efficiently as it should. This leads to fatigue, fluid buildup in the legs, and reduced oxygen delivery to muscles and the brain. Seniors with heart failure often experience leg weakness and breathlessness, making it much harder to stay steady on their feet.
A sturdy walker can provide critical support in these moments. See our Safest Walkers for Seniors: Top 5 Secure and Sturdy Choices for reliable options.
4. Coronary Artery Disease (CAD)
Coronary artery disease restricts blood flow to the heart, often causing fatigue and reduced physical capacity.
As seniors with CAD tire more easily, their muscle coordination and reaction time decrease, both of which are critical for preventing falls.
5. Cardiac Medications and Their Side Effects
Many medications used to manage heart conditions, including beta-blockers, diuretics, and blood pressure drugs, can cause side effects that increase fall risk.
These include dizziness, fatigue, dehydration, and low blood pressure. Seniors managing multiple prescriptions should review their medications regularly with their doctor.
The Role of Diet in Heart Health and Fall Risk
What seniors eat directly affects their heart health, and by extension, their fall risk. A diet high in sodium, saturated fats, and processed foods can worsen cardiovascular conditions and contribute to instability.
Proper footwear also plays a role in reducing fall risk. Read our guide on Why Seniors Need Proper Walking Shoes for practical recommendations.
How to Reduce Fall Risk if You Have Heart Issues
Strategy
| How It Helps
|
Warning Signs to Watch For
If you or a loved one has a heart condition, be alert to these signs that could indicate an increased fall risk:
- Sudden dizziness or lightheadedness, especially when standing up
- Unexplained fatigue or weakness in the legs
- Heart palpitations or a racing heartbeat before or during activity
- Shortness of breath during light activity or walking
- Brief episodes of confusion or disorientation
These symptoms should always be reported to a doctor immediately. In the meantime, having a reliable mobility aid on hand can provide critical support. Our guide on Best Mobility Devices for Seniors covers a wide range of options to suit different needs.

Tips for Caregivers Supporting Seniors with Heart Conditions
Caring for a senior with heart issues requires extra awareness around fall prevention. Here are some practical steps:
- Ensure the home is fall-proof: Remove loose rugs, improve lighting, and install grab bars in bathrooms.
- Encourage slow position changes: Help seniors stand up gradually to prevent orthostatic hypotension.
- Review medications regularly: Work with the senior’s doctor to identify any drugs that may increase fall risk.
- Choose the right mobility aid: A rollator or upright walker can provide stability during dizzy spells.
- Have an emergency plan: Learn what to do in a fall situation
Frequently Asked Questions
Can a heart condition directly cause a fall?
Heart conditions like arrhythmia and orthostatic hypotension can cause sudden dizziness, fainting, or weakness that directly leads to falls. Managing your heart condition actively is one of the best ways to reduce this risk.
What heart medication is most associated with falls in seniors?
Diuretics and blood pressure medications are most commonly linked to falls because they can cause dehydration and low blood pressure. Always discuss side effects with your doctor and never stop taking prescribed medication without medical advice.
Should seniors with heart conditions use a walker?
In many cases, yes. A walker provides stability during episodes of dizziness or weakness.
Can exercise help reduce fall risk for seniors with heart disease?
Gentle, doctor-approved exercise can strengthen the heart and improve balance. Always consult your physician before starting any new exercise routine.
-
Final Thoughts
Heart health and fall prevention are more closely connected than most people realize. By understanding how heart conditions affect balance, blood pressure, and energy levels, seniors and their caregivers can take proactive steps to reduce risk.
The right combination of medical care, proper nutrition, appropriate mobility aids, and home safety measures can make a significant difference in quality of life.
-
References
- Centers for Disease Control and Prevention (CDC). Older Adult Falls. https://www.cdc.gov/falls/about/index.html
- American Heart Association. Heart Failure and Fall Risk in Older Adults. https://www.heart.org/en/health-topics/heart-failure
- National Institute on Aging. Falls and Older Adults. https://www.nia.nih.gov/health/falls-and-older-adults
- Mayo Clinic. Orthostatic Hypotension: Symptoms and Causes. https://www.mayoclinic.org/diseases-conditions/orthostatic-hypotension
- Journal of the American Geriatrics Society. Cardiovascular Conditions and Fall Risk. https://agsjournals.onlinelibrary.wiley.com




